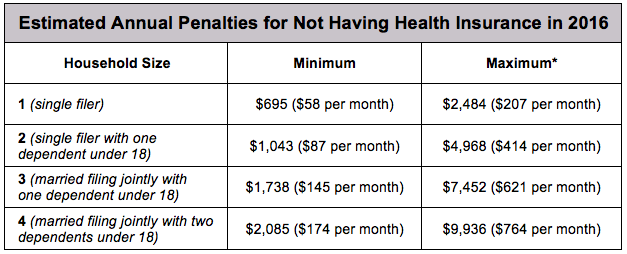
Tax bill will not seek repeal of individual health insurance mandate
The Hill- BY PETER SULLIVAN - 11/02/17 09:51 AM EDT The tax reform bill to be released Thursday will not include a repeal of ObamaCare's individual mandate, sources say, despite President…